Apicoectomy
What is an Apicoectomy and Why Should I Have One?
Sometimes a tooth that has had endodontic treatment (a root canal procedure) fails. This can happen soon after the procedure or many years following it. The failure of an endodontically treated tooth can lead to pain, swelling or both. A patient in this situation has several alternatives: non-surgical endodontic re-treatment (basically, the “re-doing” of a root canal procedure); tooth extraction and replacement with a bridge or implant; or an apicoectomy. An apicoectomy can help retain the tooth for an indefinite time period. It is a minor surgical procedure with many advantages over tooth extraction followed by an implant.
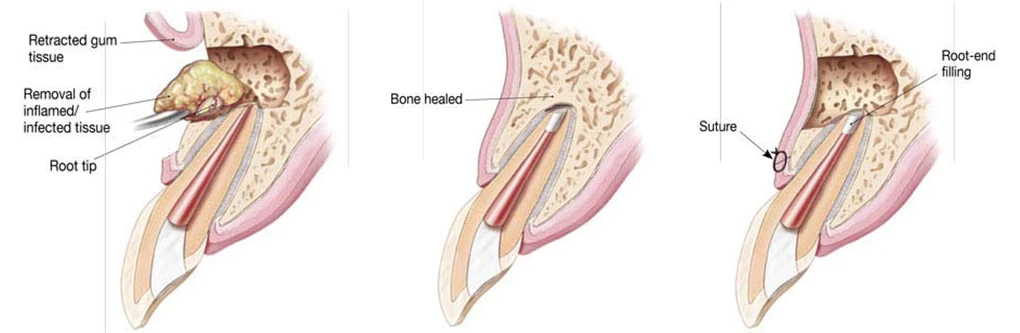
Root canal treatment is a dental procedure to remove inflamed or infected pulp on the inside of the tooth which is then carefully cleaned and disinfected, then filled and sealed. Root canal treatment is designed to eliminate bacteria from the infected root canal, prevent reinfection of the tooth and save the natural tooth.
Endodontic treatment helps you maintain your natural smile, continue eating the foods you love and limits the need for ongoing dental work. With proper care, most teeth that have had root canal treatment can last a lifetime.
Over a period of months, the bone heals around the end of the root.
Careful follow-up examinations and dental x-rays will confirm that proper healing has occurred. Follow-up visits are scheduled as necessary.
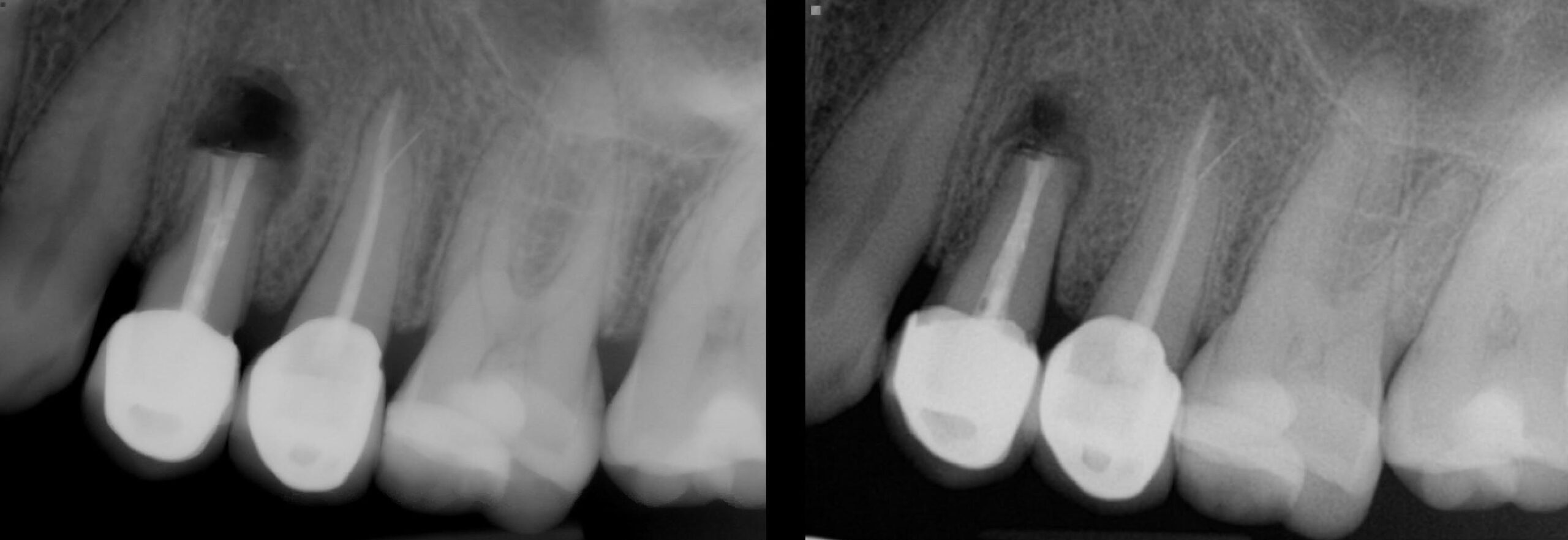
Actual “Before and After” X-rays
Patient’s tooth with previous endodontic treatment failing. Note the bone loss at the end of the roots which is indicative of a periapical infection.
The ends of the roots (apices) have been shortened, the bone has been manually cleaned and the ends of the roots have been filled or plugged with a biocompatible filling. This will help the bone regenerate.